Spirometry, as an objective measure of how an individual inhales and exhales air as a function of time is the gold standard for diagnosis, assessing and monitoring COPD. The Forced Expiratory Volume in the first second of maximal expiration after a miximal inspiration (FEV1) is used to assess the severity of COPD and is a marker of disease progression.
Stages Of COPD
Mild airflow limitation (FEV1/FVC < 70%; FEV1 ≥ 80% predicted) and sometimes, but not always chronic cough and sputum production.Stage 2: Moderate COPD:Patients typically seek medical attention at this stage because of chronic respiratory symptoms or an exacerbation of their disease.
Worsening airflow limitation (FEV1/FVC < 70%; FEV1 50% to 80% predicted), with shortness of breath typically developing on exertion.Stage 3: Severe COPD:Further worsening of airflow limitation (FEV1/FVC < 70%; FEV1 30% to 50% predicted), greater shortness of breath, reduced exercise capacity, and repeated exacerbations which have an impact on a patient’ quality of life.Stage 4: Very severe COPD:
At this stage, quality of life is very appreciably impaired and exacerbations may be life-threatening
Severe airflow limitation (FEV1/FVC < 70%; FEV1< 30% predicted or FEV1 < 50% predicted plus chronic respiratory failure).
Figure 1 shows the difference in spirometry results between a person with normal lungs and one with COPD.
Graph Spirometry
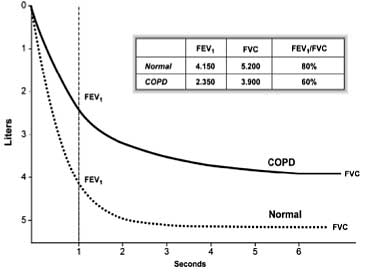
Normal spirometry result versus a COPD result
- FVC (Forced Vital Capacity): maximum volume of air that can be exhaled during a forced manoeuvre.
- FEV1 (Forced Expired Volume in one second): volume expired in the first second of maximal expiration after a maximal inspiration.
- FEV1/FVC: FEV1 expressed as a percentage of the FVC, gives a clinically useful index of airflow limitation.
- The ratio FEV1/FVC is between 70% and 80% in normal adults; a value less than 70% indicates airflow limitation and the possibility of COPD.
